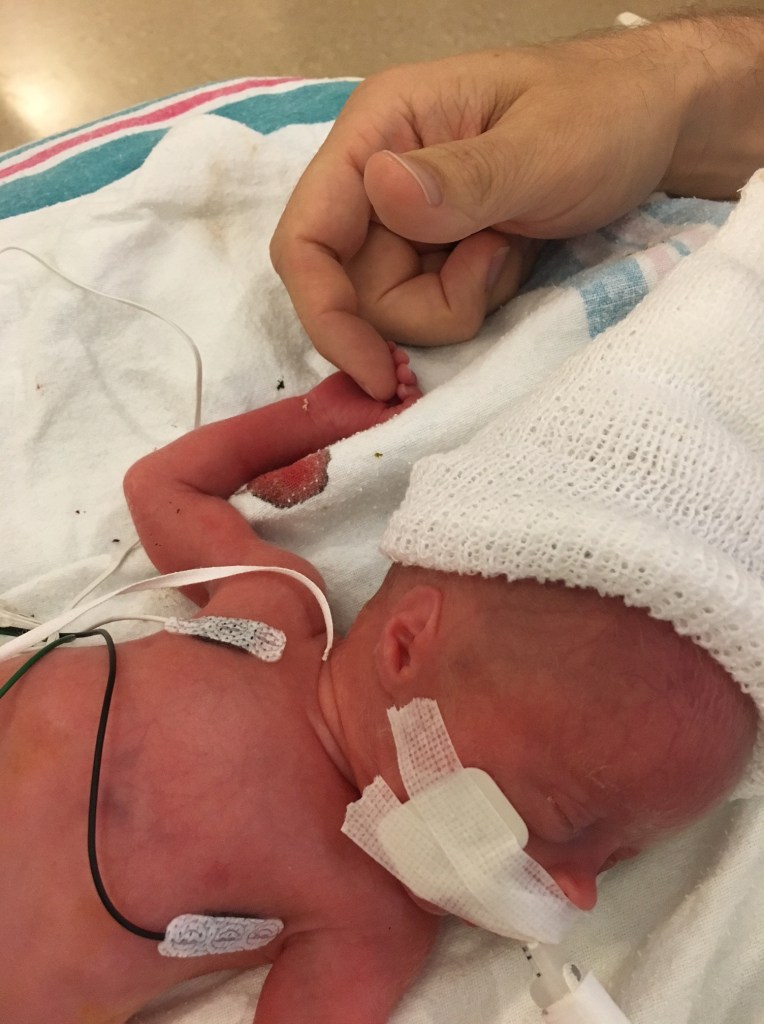
Emmett is now about 34 hours old and we are learning all there is to know about milestones, life in the NICU and a bunch of other stuff I never thought I’d need to know. I’m going to do my best to keep this blog updated with Emmett’s progress and things we’re learning, even if some of the details may be a bit fuzzy to me. As you can imagine, my head is currently spinning.
Honeymoons and two-steps:
When we arrived yesterday, the doctors and NICU staff warned us right off the bat that the first 24 hours in the NICU tend to be the honeymoon period, and that going forward, it’s common for things to take a “two steps forward, one step back” pattern, even in the best of cases. So we’re learning to strike a balance between positive thinking and realism. That said, everyone has been marveling at how well Emmett has been doing so far!
Goals and milestones:
Long-term (i.e., in order to spring him from this joint), our big milestones we have to hit are: breathing on his own, regulating his temperature on his own, sleeping in a crib and not an incubator (I think this is related mostly to temperature regulation) and all feedings via mouth (breast or bottle, as opposed to IV or tube). There are many, many smaller milestones and sub-milestones, but those are the biggies.
Progress report:
I’m happy to report, E is already making great progress on the breathing front. When he was born, they had to immediately intubate him and hook him up to a respirator that breathes for him. According to the doctors, babies this premature get easily tired and basically forget to breathe. So he has to learn to do it on his own. Earlier today they were able to stop the continuous forced breathing and instead set him up so if he didn’t take a breath every two seconds, the machine would kick on for him and help him. Later this afternoon, they increased that interval to four seconds. They’re basically testing his ability to do it himself by offering less and less help (but always having safeguards in case he doesn’t take a breath on his own). He’s been doing great, and if he continues to do well throughout the night, they will actually remove the breathing tube tomorrow morning (which will allow us to see more of his beautiful face and actually hear him cry!), and put him on a CPAP or a forced-air cannula. These will still offer some assistance and not let him go without oxygen if he were to forget to breathe, but they both allow for a little more independence. They’ve cautioned us that if he doesn’t do as well on that as they’d hoped, there’s always a chance we could have to go back to the breathing tube (again – two steps forward, one step back), but at this point they’re feeling optimistic he can do it.
There’s also a chance tomorrow that they may be able to remove the catheters that are inserted in his belly button that are measuring his blood oxygen level (I think? My head is swimming) sugars and blood gases (just confirmed), and if that happens, we may even get to hold him and do skin-to-skin for the first time. We can hold him with most of his tubes and wires still hooked up, but the belly button ones are particularly fragile, so those have to come out first.
I’m happy to report his bilirubin levels have been pretty good and he isn’t showing signs of jaundice. So no phototherapy needed yet, but that doesn’t mean he won’t need it at some point. It’s still early.
Random learnings:
It’s past midnight now and after just four hours of sleep last night, I think the adrenaline may finally be surrendering to the fatigue, so I’m going to wrap this post with a random brain dump of just a few of the many things we’ve learned about life in the NICU. It’s a whole ‘nother world, for sure…
- You will wash your hands raw. Enter a room? Leave a room? Eat? Touch your face or hair? You wash your hands before you do anything and everything. I got an amazing care package from some dear friends yesterday and they thought to include hand lotion. Smart.
- It’s hard not to jump every time you hear an alarm. And there are a lot of alarms.
- You do start to learn the difference between the really bad alarms (heart or breathing-related, etc.) and the more innocuous ones (for example, the IV station monitor alerts when a bag is half full, then 1/4 full, and then empty. We get it, IV.).
- In addition to the alarms in your own room, the monitors in the hallway have alarms for all the patients for safety redundancy, and since doors are almost always open for easy staff access, it’s sometimes hard to tell whether the sound is coming from your room or the hallway. And then you feel relief, followed by guilt for feeling relieved, when you realize it’s not your baby’s alarm that’s sounding.
- The NICU staff are truly amazing. I’m already in love with our doctors, nurses and respiratory therapists and we’ve only been here a day. I can already tell leaving them will be a bittersweet and emotional experience. I can only imagine the types of heartbreaking situations these folks deal with on a regular basis. On top of that, they patiently explain everything to parents like me who hover over their shoulder and ask them millions of questions while they’re trying to do their job.
- Trying to get your milk to come in via pumping instead of nursing SUCKS. Especially when your boobs thought they had another 14 weeks before they had to perform.
- There’s a lot of downtime. We have been told we can touch Emmett when he’s awake, but to let him sleep as much as possible. So for a lot of the day, we’re just sitting here. I’ve kept myself busy keeping friends and family updated, but even if I’m not interacting with E directly, it’s still comforting to just be here beside him. If (God forbid) something went wrong, I would want to be here, and I also want to be here to celebrate every milestone and achievement.
- There’s a certain solidarity between NICU families. Whether it’s a weary smile from another parent in the hallway or an email or text from a friend who’s been there (or a friend of a friend, in some cases!), I’m finding a rapidly growing network of others who just get it. Some of the best “therapy” for me so far has been simply hearing success stories of children who got a rough start way too early but are thriving now. There’s actually a wall in the hallway here with photos of beautiful, smiling children of various ages. Under each one is a plaque that states their weight and gestational age at birth. It’s truly beautiful, and brings a smile to my face every time I walk by.